Measles booster
Measles has been “eliminated” in the U.S. for a quarter century. That means an entire generation grew up with little risk of exposure. Inevitably, vaccination rates dropped, and post-COVID rates are below the threshold for herd immunity. If you’re over 35, you may have received an early vaccine protocol with less protection than is available today, and you may want to ask your doctor about a booster shot.
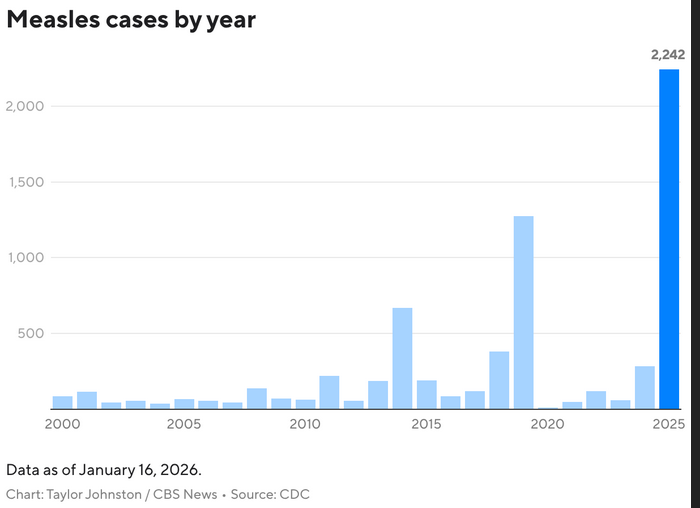
Why we do it:
Measles is an incredibly contagious, airborne disease. The U.S. has occasionally had a few cases picked up from international travelers, but for 25 years, high levels of vaccination kept those outbreaks small. New infections burned out quickly and risk of exposure remained small.
Today that’s no longer true. Each disease has a herd immunity threshold, based on how contagious it is. This is the point at which a pocket of infection will burn out, rather than spread. For measles, 95% of the population must be immune, either through prior infection or through vaccination. In some counties in the U.S. the number is closer to 60% now. That means one exposure leads to many new cases.
Measles isn’t just a dangerous and miserable disease, it also causes your immune system to forget how to fight other diseases. This immune amnesia leads to increased risk of death for years after infection.
This is not a uniquely American problem: vaccine skepticism is spreading worldwide, but that makes the situation worse, not better. If you are older than 35, you may want to get a booster. Whether you need one depends on your risk tolerance and vaccine history.
If you were born after 1989 and vaccinated, you’re all good!
If you are 37-55, you likely received 1 MMR shot, with 93% immunity. Two doses give close to 100% protection, and a booster is recommended if you are high-risk, or simply want more protection.
If you are 55-62, you will need to know your specific vaccination type to determine if you need a booster or you can request an antibody test. This article breaks it down.
If you are over 62, you were not vaccinated as a child, but may have had measles, or may have been vaccinated due to military service, travel or employment. You should talk to your doctor.
If you served in the military, check this chart for vaccination protocols by year.
If you are unsure of your disease or vaccination history, you can ask your doctor for a titer to test for immunity.
If you are being treated for certain illnesses that suppress immunity, including some cancers and auto-immune diseases, measles is an attenuated vaccine (live but weak) and may not be recommended for you. Consult your doctor.



